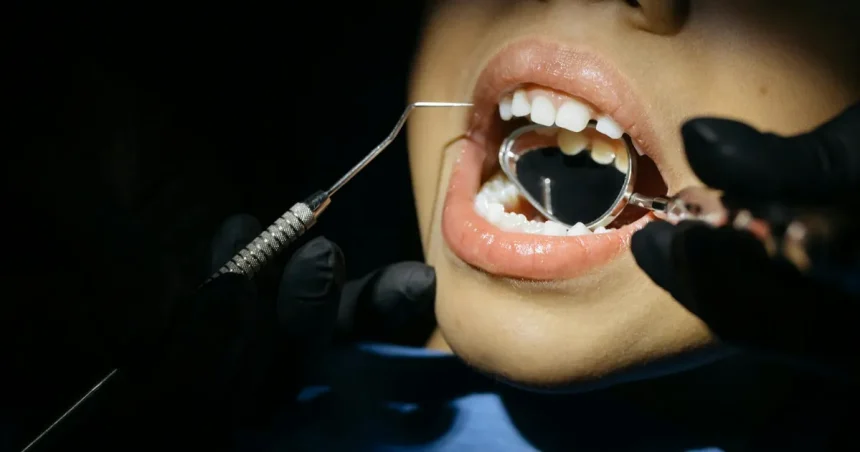
Tooth decay doesn’t announce itself with a grand entrance—it creeps in quietly, often disguised as minor discomfort or a fleeting twinge. Yet ignoring these early signs can lead to painful cavities, infections, or even tooth loss. Recognizing the subtle (and not-so-subtle) warnings of tooth decay early can save you from costly dental procedures and preserve your smile. Whether it’s a persistent ache after sipping cold water or a mysterious stain on your enamel, your teeth are sending signals you shouldn’t dismiss. This guide uncovers the most overlooked signs of tooth decay, explains why they matter, and reveals what to do next—before a small issue becomes a dental emergency.
What Is Tooth Decay? A Quick Definition
Tooth decay, also called dental caries, is a progressive breakdown of your tooth’s structure caused by acids produced by bacteria in plaque. These acids erode the enamel—the hard, protective outer layer—creating tiny holes (cavities) that deepen over time. Left untreated, decay can reach the inner pulp, triggering infections, abscesses, and severe pain. It’s one of the most common chronic diseases worldwide, yet entirely preventable with proper care. Understanding its early signs is your first line of defense.
Persistent Tooth Sensitivity: More Than Just a Nuisance
That sharp, sudden jolt when you bite into ice cream or sip hot coffee? It’s not just a quirk—it’s often your tooth’s way of sounding the alarm. Sensitivity to temperature extremes is one of the earliest and most common signs of tooth decay. When enamel wears down, the underlying dentin (a porous layer filled with tiny nerve endings) becomes exposed. Cold, heat, or even sweet foods can trigger discomfort as these nerves react to stimuli.
But not all sensitivity is created equal. Occasional twinges might stem from receding gums or aggressive brushing, but persistent sensitivity—especially in one specific tooth—usually signals decay. If the pain lingers for more than a few seconds after removing the trigger, it’s time to schedule a dental checkup. Ignoring it could mean the decay has already progressed to a cavity or worse, an infection.
When Sensitivity Signals a Bigger Problem
Sensitivity that worsens at night or disrupts sleep is particularly concerning. This often indicates the decay has reached the tooth’s pulp, where nerves and blood vessels reside. At this stage, a simple filling may no longer suffice—you might need a root canal to save the tooth. Another red flag? Sensitivity that occurs without an obvious trigger, like spontaneous pain. This suggests advanced decay or even an abscess, which requires immediate attention.
How to Differentiate Sensitivity from Other Issues
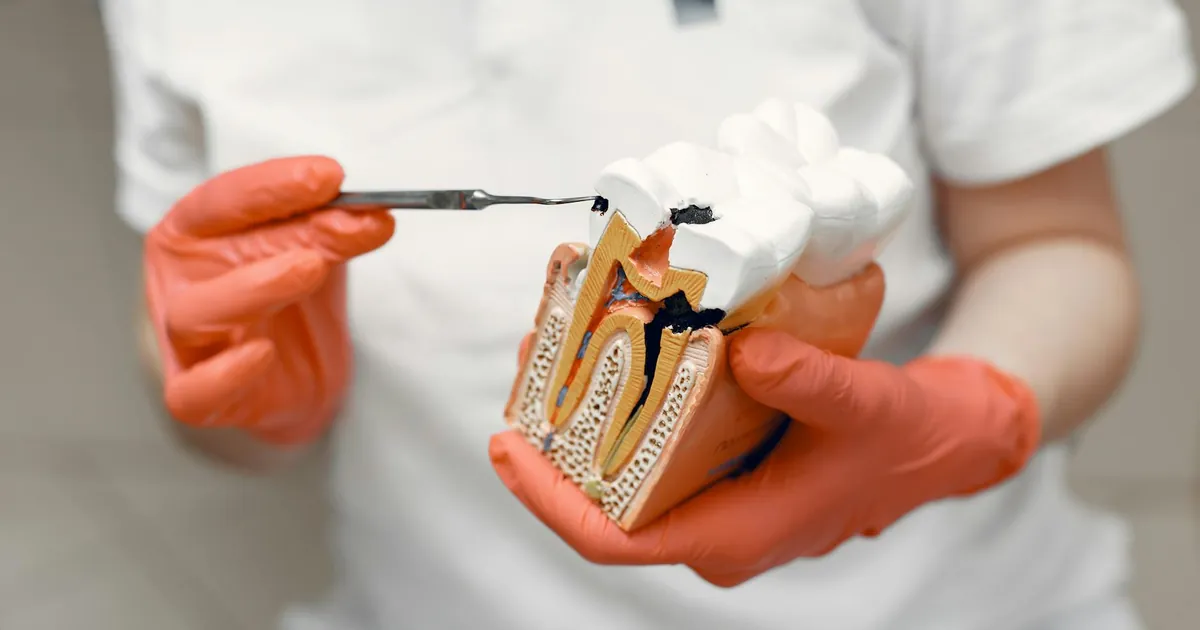
Not all tooth pain is decay-related. Gum disease, cracked teeth, or even sinus infections can mimic sensitivity. A quick test: Does the pain occur only when eating or drinking, or does it happen randomly? Does it affect multiple teeth or just one? If it’s localized and tied to specific triggers, decay is the likely culprit. For a deeper dive into tooth pain causes, check out this related article on quick relief tips.
Visible Stains or Discoloration: The Silent Clues
Your teeth aren’t supposed to look like a patchwork quilt. While some staining is normal (thanks, coffee and red wine), certain discolorations are dead giveaways for decay. White spots, for instance, often appear in the early stages of enamel demineralization. These chalky patches signal that acids are leaching minerals from your tooth, weakening its structure. Over time, they can turn brown or black as the decay progresses.
Brown or black spots are even more alarming. They typically indicate that a cavity has already formed, and the decay is actively eating away at your tooth. Unlike superficial stains from food or tobacco, these spots won’t brush away. They may also feel rough or sticky to the touch—a sign that plaque has hardened into tartar, further fueling the decay process.
Types of Stains and What They Mean

Not all stains are equal. Here’s a quick breakdown:
- White spots: Early decay or fluorosis (excess fluoride exposure).
- Brown spots: Moderate decay or tartar buildup.
- Black spots: Advanced decay or dead tooth tissue.
- Yellowish stains: Often surface-level, but can indicate thinning enamel.
If you notice any of these, don’t wait for the stain to “go away.” A dentist can determine whether it’s decay or something less serious, like a harmless pigmentation issue.
Why You Shouldn’t Ignore Even Small Stains
It’s easy to dismiss a tiny brown spot as “no big deal,” but decay doesn’t work that way. Once bacteria breach the enamel, they multiply rapidly, creating a cavity that grows deeper and wider. What starts as a pinprick can become a gaping hole in months. Worse, decay can spread to adjacent teeth, turning a minor issue into a full-blown dental disaster. Regular checkups can catch these spots early, often before they require anything more than a simple filling.
Bad Breath or a Foul Taste: The Hidden Red Flags
Chronic bad breath (halitosis) isn’t just embarrassing—it can be a sign of tooth decay or gum disease. When bacteria feast on food particles and plaque, they release sulfur compounds that smell like rotten eggs. If your breath doesn’t improve with brushing, flossing, or mouthwash, decay might be the culprit. Similarly, a persistent foul taste in your mouth—especially near a specific tooth—can indicate an infection or abscess.
These symptoms often fly under the radar because people assume they’re temporary or diet-related. But if you notice a metallic, bitter, or sour taste that lingers for days, it’s worth investigating. Decay creates pockets where food and bacteria get trapped, leading to odor and taste issues. The longer you ignore it, the worse it gets—and the harder it becomes to treat.
How Decay Causes Bad Breath
Here’s the science: Bacteria in your mouth break down sugars and starches, producing acids that erode enamel. As the decay progresses, it creates tiny crevices where food debris and bacteria accumulate. These pockets become breeding grounds for odor-causing microbes. Unlike surface-level bad breath, which can be masked with mints, decay-related halitosis requires professional cleaning and treatment to resolve.
When to See a Dentist About Bad Breath
If you’ve ruled out dietary causes (like garlic or onions) and your bad breath persists despite good oral hygiene, it’s time to see a dentist. Other warning signs include:
- A white or yellow coating on your tongue.
- Swollen or bleeding gums.
- A constant dry mouth (which reduces saliva’s natural cleaning action).
A dentist can identify whether decay, gum disease, or another issue is to blame and recommend the right treatment.
Pain When Chewing: A Warning You Can’t Chew Over
If biting into an apple or crunching on chips sends a jolt of pain through your tooth, don’t chalk it up to “sensitivity.” Pain while chewing is a classic sign of advanced tooth decay, a cracked tooth, or an abscess. When decay reaches the inner layers of your tooth, it can cause inflammation or even expose the nerve, making every bite excruciating.
This type of pain is often sharp and localized, meaning you can pinpoint exactly which tooth is affected. It might also come and go, lulling you into a false sense of security. But here’s the hard truth: If a tooth hurts when you chew, the problem isn’t going away on its own. In fact, it’s likely getting worse. The longer you wait, the more invasive (and expensive) the treatment becomes.
Why Chewing Pain Is a Dental Emergency

Chewing pain usually indicates one of three things:
- Advanced decay: The cavity has reached the dentin or pulp, causing inflammation.
- Cracked tooth: Decay weakens the tooth, making it prone to fractures.
- Abscess: A pocket of pus has formed at the tooth’s root, causing pressure and pain.
All three scenarios require prompt treatment. An abscess, in particular, can spread infection to your jaw, sinuses, or even your bloodstream if left untreated. If your tooth hurts when you chew, call your dentist immediately—don’t wait for the pain to become unbearable.
How to Manage Chewing Pain at Home
While you wait for your dental appointment, you can take steps to ease the discomfort. Avoid hard, crunchy, or sticky foods that aggravate the tooth. Stick to soft foods like yogurt, mashed potatoes, or smoothies. Over-the-counter pain relievers like ibuprofen can help reduce inflammation, but don’t rely on them as a long-term solution. For more tips on managing tooth pain, check out this guide on quick relief.
Swollen or Bleeding Gums: The Overlooked Connection
Gums that bleed when you brush or floss are often dismissed as a sign of “brushing too hard.” But if your gums are consistently swollen, red, or tender, it could be a sign of gum disease—or worse, tooth decay spreading below the gumline. Decay doesn’t just affect the visible parts of your teeth. When bacteria reach the roots, they can infect the surrounding gum tissue, leading to inflammation, bleeding, and even gum recession.
This is especially true for cavities near the gumline. These “root cavities” are harder to spot and treat because they’re hidden beneath the gums. They also progress faster than cavities on the chewing surfaces, as the root’s surface (cementum) is softer than enamel. If your gums are bleeding and you notice other signs of decay, like sensitivity or bad breath, don’t assume it’s just gingivitis. It could be a double whammy of decay and gum disease.
How Decay Leads to Gum Problems
Here’s how it happens: Decay creates a rough surface where plaque and bacteria accumulate. Over time, this irritates the gums, causing them to pull away from the tooth. The resulting pockets trap more bacteria, leading to infection and inflammation. If left untreated, this can progress to periodontitis, a severe form of gum disease that can destroy the bone supporting your teeth.
When to Worry About Bleeding Gums
Occasional bleeding during flossing isn’t usually a cause for concern. But if your gums bleed every time you brush or floss, or if they’re swollen and tender for more than a week, it’s time to see a dentist. Other red flags include:
- Gums that recede or pull away from your teeth.
- Pus between your teeth and gums.
- A persistent bad taste in your mouth.
These symptoms often indicate advanced decay or gum disease, both of which require professional treatment.
Pits or Holes in Your Teeth: The Obvious (But Often Ignored) Sign
If you run your tongue over your teeth and feel a rough spot or a tiny hole, congratulations—you’ve found a cavity. Pits or holes are the most obvious signs of tooth decay, yet many people ignore them, assuming they’re too small to matter. But here’s the thing: Cavities don’t heal on their own. Once a hole forms, it will only get bigger, deeper, and more painful over time.
These holes often start as small, barely noticeable pits. You might not feel any pain at first, which is why they’re so easy to overlook. But as the decay progresses, the hole grows, exposing more of the tooth’s inner layers. Eventually, you’ll start to feel sensitivity, pain, or even a sharp edge that catches food. By then, the cavity has likely reached the dentin or pulp, requiring more extensive treatment.
Why Small Holes Are a Big Deal
A tiny hole might seem harmless, but it’s a gateway for bacteria. Every time you eat or drink, food particles get trapped in the cavity, feeding the bacteria and accelerating the decay. Over time, the hole expands, weakening the tooth’s structure. If the decay reaches the pulp, you’ll need a root canal to save the tooth. In severe cases, the tooth may need to be extracted.
How to Check for Cavities at Home
While you can’t diagnose cavities yourself, you can look for warning signs. Run your tongue over your teeth—do you feel any rough spots, pits, or holes? Use a small mirror to inspect hard-to-see areas, like the back molars. If you notice anything unusual, schedule a dental appointment. A dentist can confirm whether it’s a cavity and recommend the best course of action.
Key Takeaways: Don’t Ignore These Signs
- Tooth sensitivity to hot, cold, or sweet foods is often the first sign of decay.
- White, brown, or black spots on your teeth can indicate early to advanced decay.
- Persistent bad breath or a foul taste may signal an infection or abscess.
- Pain when chewing is a red flag for advanced decay, cracks, or abscesses.
- Swollen, bleeding gums can be a sign of decay spreading below the gumline.
- Pits or holes in your teeth are cavities that won’t heal on their own.
- Regular dental checkups can catch decay early, before it becomes a major problem.
Expert Insights: What Dentists Want You to Know
“Many patients wait until they’re in excruciating pain to see a dentist, but by then, the decay has often progressed to a point where treatment is more invasive and costly. The key is to act at the first sign of trouble—whether it’s sensitivity, a stain, or a rough spot. Early intervention can save your tooth and your wallet.”
Frequently Asked Questions
Can tooth decay go away on its own?
No. Tooth decay is a progressive condition that requires professional treatment. While early demineralization (white spots) can sometimes be reversed with fluoride treatments and improved oral hygiene, once a cavity forms, it won’t heal without a filling or other dental intervention.
How quickly does tooth decay progress?
It depends on several factors, including your diet, oral hygiene, and genetics. In general, decay can progress from a small white spot to a cavity in as little as 6 months. Without treatment, a cavity can reach the pulp within 1–2 years, leading to infection and potential tooth loss.
Are there home remedies to stop tooth decay?
While home remedies like oil pulling or fluoride rinses can help slow decay, they can’t reverse cavities. The best way to stop decay is to visit a dentist for a filling, crown, or other treatment. Maintaining good oral hygiene—brushing twice daily, flossing, and using fluoride toothpaste—can prevent new cavities from forming.
Why does my tooth hurt at night but not during the day?
Nighttime tooth pain often indicates advanced decay or an abscess. When you lie down, blood flow to your head increases, putting pressure on the inflamed nerve in your tooth. This can cause throbbing pain that disrupts sleep. If you experience this, see a dentist as soon as possible—it’s a sign the decay has reached a critical stage.
Can a cavity cause headaches or earaches?
Yes. Decay in your molars can radiate pain to your jaw, ears, or even your head. This is called “referred pain,” where the brain misinterprets the source of the discomfort. If you have unexplained headaches or earaches, especially on one side of your face, a dental issue could be the culprit.
Is it normal for a filling to hurt after the procedure?
Mild sensitivity after a filling is normal and should subside within a few days. However, if the pain is sharp, persistent, or worsens over time, it could indicate a problem, such as an improperly placed filling, a cracked tooth, or an infection. Contact your dentist if the pain doesn’t improve.
How can I prevent tooth decay naturally?
Preventing decay starts with a healthy diet and good oral hygiene. Limit sugary and acidic foods, which feed bacteria and erode enamel. Drink plenty of water to rinse away food particles and bacteria. Chew sugar-free gum to stimulate saliva, which neutralizes acids. And don’t skip your dental checkups—professional cleanings remove plaque and tartar that brushing can’t reach.
Tooth decay is sneaky, but it’s not invincible. By recognizing the early signs—sensitivity, stains, bad breath, pain, or holes—you can take action before a small problem becomes a dental disaster. Don’t wait for the pain to become unbearable. Schedule a checkup today, and give your teeth the care they deserve. Your future self (and your smile) will thank you.